
NEW! Listen to this blog by pressing the “Play” button below!
VA Disability Rating for PTSD: Criteria, Eligibility, and Making a Strong Disability Claim
There are many different events that cause PTSD (Post-traumatic Stress Disorder). Some examples are personal trauma, sexual trauma, combat (see: combat veterans), and reactions to training. This condition is the 6th most-rated disability among veterans. There were over 63,000 new claims in 2015, and the VA compensates more than 800,000 veterans for symptoms of PTSD at some level.
When a veteran can show that their PTSD is service connected, the VA will assign a disability rating. A disability rating is based on the earnings lost due to the PTSD. The VA will use medical evidence to determine the severity of the disability.
The VA will nearly always require a C&P exam. It is important to note that C&P examiners do not rate claims. Exam results go to a VA adjudicator to apply the rating formula and provide a rating for the veteran’s PTSD.
When the VA is evaluating a PTSD claim, it looks to both the rating formula and the DSM-V. In evaluating ratings, the VA can consider factors outside of the rating schedule. However, the DSM-V symptoms are not meant to replace, but supplement, the rating formula scale for PTSD. Additionally, the rating formula factors for PTSD are examples of severity of the condition, not an exhaustive list.
This guide will break down the general rating formula for mental health conditions, the rating formula for PTSD specifically, and how veterans can best make a claim for VA disability benefits.
Below is our Ultimate Video Guide for PTSD.
If you would like to skip to our Ratings section in the Ultimate Video Guide for PTSD, please skip to Chapter 25.
Understanding The General Rating Formula for Mental Health Conditions
Before diving into the VA’s rating system for PTSD, it’s important to understand their general rating formula for mental disorders. Disclaimer, VA actually rates every mental health condition under the same General Rating Formula and rating criteria. The only exception being PTSD and needing to prove PTSD stressors. Symptoms are then assigned a disability rating.
PTSD disability ratings can be 10%, 30%, 50%, 70%, or 100%. Transparency about your worst symptoms is vital for your rating. VA often rates veterans by the average of their symptoms. So, if a veteran has such symptoms that fall in the 30, 50, and 70% PTSD rating ranges, they will often get a 50% PTSD rating. However, this is not the correct way to rate a mental health disorder.
The basis of a rating SHOULD BE the highest level of symptoms, not an average. So, if a veteran has six symptoms at 30%, three at 50%, and two at 70%, a 70% PTSD rating is proper. Also, the VA cannot downplay symptoms and give the veteran a lower PTSD rating or whichever mental health condition is more severe.
For example, if a veteran has suicidal ideations, that is a 70% PTSD rating. However, VA doctors sometimes state that the veteran does not have intent or that the ideations are fleeting. The VA will sometimes grant a lower rating by minimizing the symptom altogether. It is, nevertheless, a 70% PTSD rating if a veteran has suicidal ideations—no matter the frequency or intent.
One rating not on the PTSD scale is Total Disability Based on Individual Unemployability (TDIU, also known as IU). PTSD often causes veterans to not be able to work. VA calls this IU. If your PTSD causes IU you should file for that as well. It is basically another way to get 100% benefits.
Do you want to learn about how to increase your VA rating for PTSD?
Know that there are many secondary conditions for PTSD you may not be aware of.
Check out our guide for more info!
Understanding VA PTSD Ratings

The VA rating formula goes from zero percent to 100 percent in increments of 10. Not every disability includes each rating percentage. For example, a veteran’s PTSD can be rated at 0, 10, 30, 50, 70, or 100 percent debilitating.
A zero percent rating means that “PTSD has been diagnosed. The symptoms, however, are not severe enough to interfere with work or social functioning or to require continuous medication.” A 100% rating is for “total occupational and social impairment” due to specified symptoms.
What if the veteran cannot work due to post-traumatic stress disorder?
Another way to earn a 100% PTSD rating is for the veteran to receive unemployability (IU) for his PTSD. Unemployability is not on the PTSD rating schedule. IU is a way for the veteran to receive 100% without meeting all the requirements on the 100% rating.
The VA grants IU ratings when a veteran cannot work due to his service-connected disabilities. When the VA gives an Unemployability rating for PTSD, it means a veteran cannot work due to his PTSD. As a result, a veteran receives a 100% PTSD rating due to unemployability.
| General Rating Formula for Mental Disorders | Rating |
|---|---|
| Total occupational and social impairment, due to such symptoms as: gross impairment in thought processes or communication; persistent delusions or hallucinations; grossly inappropriate behavior; persistent danger of hurting self or others; intermittent inability to perform activities of daily living (including maintenance of minimal personal hygiene); disorientation to time or place; memory loss for names of close relatives, own occupation, or own name. | 100 |
| Occupational and social impairment, with deficiencies in most areas, such as work, school, family relations, judgment, thinking, or mood, due to such symptoms as: suicidal ideation, obsessional rituals which interfere with routine activities; speech intermittently illogical, obscure, or irrelevant; near-continuous panic or depression affecting the ability to function independently, appropriately and effectively; impaired impulse control (such as unprovoked irritability with periods of violence); spatial disorientation; neglect of personal appearance and hygiene; difficulty in adapting to stressful circumstances (including work or a work-like setting); inability to establish and maintain effective relationships | 70 |
| Occupational and social impairment with reduced reliability and productivity due to such symptoms as: flattened affect; circumstantial, circumlocutory, or stereotyped speech; panic attacks more than once a week; difficulty in understanding complex commands; impairment of short – and long-term memory (e.g., retention of only highly learned material, forgetting to complete tasks); impaired judgment; impaired abstract thinking; disturbances of motivation and mood; difficulty in establishing and maintaining effective work and social relationships. | 50 |
| Occupational and social impairment with occasional decrease in work efficiency and intermittent periods of inability to perform occupational tasks (although generally functioning satisfactorily, with routine behavior, self-care, and conversation normal), due to such symptoms as: depressed mood, anxiety, suspiciousness, panic attacks (weekly or less often), chronic sleep impairment, mild memory loss (such as forgetting names, directions, recent events). | 30 |
| Occupational and social impairment due to mild or transient symptoms which decrease work efficiency and ability to perform occupational tasks only during periods of significant stress, or symptoms controlled by continuous medication | 10 |
| A mental condition has been formally diagnosed, but symptoms are not severe enough either to interfere with occupational and social functioning or to require continuous medication. | 0 |

What if a veteran exhibits symptoms of two PTSD ratings?
Where two evaluations may apply, the VA must grant the higher evaluation if the disability picture is closer to that higher rating. Otherwise, the VA will assign the lower rating. If a veteran fits criteria for both the 50% and 70% ratings, the VA should grant the 70 percent rating.
Similarly, there is the issue of IU and PTSD. If a veteran has a 70% PTSD rating and does not meet the 100% rating, his PTSD could cause IU. If that is the case, then the VA should grant 100% through IU for the PTSD.
Symptoms that the VA considers when rating PTSD include, but are not limited to:

- impairment in thought processes or communication
- grossly inappropriate behavior
- persistent danger of hurting self or others
- suicidal ideation
- intermittent inability to perform activities of daily living (including maintenance of minimal personal hygiene or self-care)
- mild memory loss
- panic attacks or depression affecting the ability to function. (PTSD and depression comorbidity)
- impaired impulse control (getting angry very quickly)
- chronic sleep impairment
- decreased work efficiency
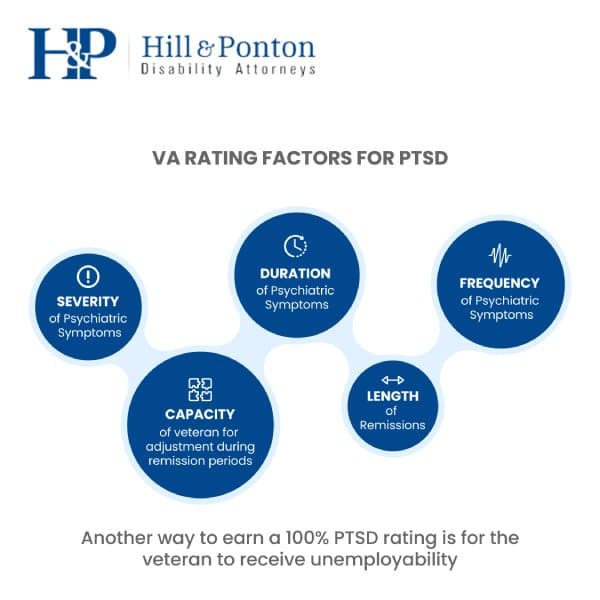
During the VA’s rater’s evaluation, they will consider multiple factors regarding symptoms:
- frequency, of psychiatric symptoms
- severity of psychiatric symptoms
- duration of psychiatric symptoms
- length of remissions
- veteran’s capacity for adjustment during periods of remission
Ready to Make a Claim? 3 Steps to Presenting a Strong VA PTSD Claim
Now that you know how the VA rates PTSD, it’s important to understand some best practices for making a claim. Keep in mind that PTSD claims can complicate the already confusing and murky claims process. Even with the new regulations passed in 2010 that make it easier for veterans with PTSD to qualify for VA benefits, a veteran with a PTSD claim will face unique challenges.
There are three requirements that make up a claim for PTSD:
- A current diagnosis
- An in-service stressor
- A link between the current diagnosis and stressor
So, you can make a strong claim by presenting these three requirements.

Step 1: Present a Current Diagnosis of PTSD
The first step to receiving VA benefits for PTSD disability requires the veteran to have a current diagnosis. A psychiatrist, psychologist, licensed social worker, or other mental health care practitioner must diagnosis the veteran with PTSD. Additionally, the diagnosis must conform to specific criteria.
It’s important that the diagnosing doctor provides a report that fully describes why they feel that the veteran has PTSD and how the veteran’s symptoms meet the specific criteria. All of this medical evidence must show that it is “as likely as not” that the veteran currently has disabling PTSD.
Step 2: Identify an In-service stressor
One of the challenges with a PTSD claim is getting service connection. PTSD is not presumed to be related to service, so a veteran needs more than just a current diagnosis. The veteran must show that the stressful event that caused PTSD occurred during service.
This does not mean that the veteran must have engaged in combat. Any traumatic event that satisfies the diagnostic criteria can be a sufficient stressor. However, there are different rules for combat vs. non-combat events. If a veteran can show that they were in combat, then a statement from the veteran may be all that is needed to prove an in-service stressor. Records that may help prove combat experience include:
- Veteran’s DD214
- Certain medals and awards received
- Unit records showing date and location of unit assignments
What other kinds of evidence can a veteran use to show an in-service event for PTSD?
On the other hand, if the veteran was not in active duty combat, he must provide more evidence than his statement alone. Sometimes the veteran’s service records can help support the veteran’s claim. But the veteran can also provide other sources of information include details about the people involved, dates, location, and a description of the event. Examples of supporting evidence include:
- Statements from fellow veterans that served with you
- Statements from family and/or friends who knew you before and after service

Step 3: Cite your Nexus for PTSD with The VA
A nexus is the link between the veteran’s current PTSD diagnosis and his in-service stressor. The veteran’s current diagnosis must be related to his in-service stressor. The veteran must prove the nexus through medical evidence, such as an opinion from a qualified doctor.
Another great resource for establishing a nexus is records from a Vet Center. Vet Centers have licensed social workers that will document the connection between the veteran’s stressor and their current diagnosis.
Keep in mind that proving each one of the three requirements above is vital to getting a PTSD claim service connected. If the proof falls short in one area, the VA will deny service connection.
What happens after VA grants service connection for PTSD?
Once a veteran establishes service connection for their PTSD claim, the battle isn’t over. The veteran must do what he can to make sure the VA gives him the correct compensation.
Compensation is based on the rating VA assigns a veteran (for example, 50%). This rating is based on how severe the veteran’s PTSD symptoms are.
Because the ratings are based on the veteran’s symptoms, it’s important to have medical records. These records should detail the symptoms the veteran suffers, and how they affect the veteran’s life.
Again, this is another area where having medical opinions is crucial to building a strong case. The max rating is 100%, but this is hard to get. A lot of veterans end up with a 70% rating and unemployability because they cannot work.
The VA will use a C&P exam to help them determine what the appropriate rating is. A veteran should review the PTSD rating criteria that VA uses. The veteran should discuss with family and friends how they see PTSD affecting the veteran. This will give the veteran evidence he needs to assure the C&P examiner as a full picture of his problems.
What About Incorrect Rating Decisions?
Often the rating decision is just incorrect. VA fails to grant PTSD cases but it also fails to consider other issues. VA denies a mental health disorder because the veteran filed for one disorder and actually has a different one.
Veterans, unless they have a doctorate in psychology, are not able to officially diagnose their own mental health disorders. Therefore, when a veteran claims PTSD, the VA can deny it. However, the VA must see if he has another condition.
The VA should determine if the veteran has another diagnosis, which it often does not do. Veterans can often avoid this process by filing a claim for a more generic issue such as “acquired psychiatric disorder.” Another option would to be to file for “service-connected mental health disorder.” By filing for benefits in this manner, the VA is responsible to diagnose and/or use medical records.
Speak to a Lawyer Who can Advocate for Your VA Claim
Receiving VA disability compensation can be complicated, so having a veterans disability attorney on your side can be helpful. Hill and Ponton is a nationwide law firm advocating for the rights of veterans everywhere.
Our lawyers have over 30 years of experience in social security disability law and we’re always ready to speak to veterans who have questions about the VA disability claims process, if they’re eligible, and what disability benefits they’re entitled to.
Click here to get a free case evaluation or call 1-888-373-9436 today.

Table of contents
- What is PTSD
- PTSD Criteria
- C&P Exam for PTSD
- PTSD Rating (current blog)
- TDIU for PTSD
- VA Decision for PTSD
- PTSD resources





