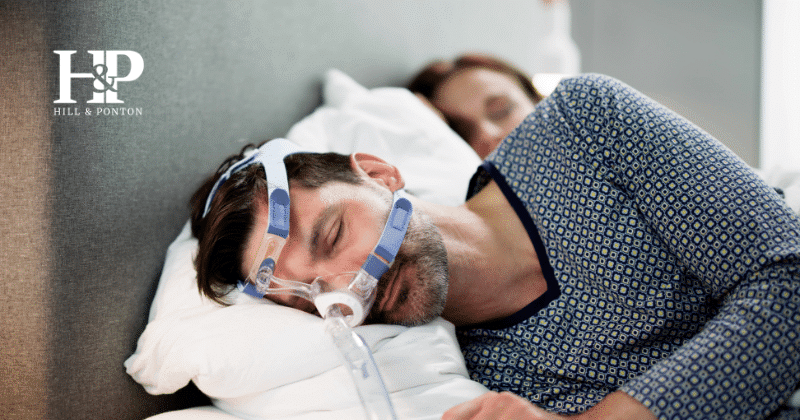
Over 500,000 veterans are recognized for sleep apnea, and more than 1.3 million for PTSD, through service-connection with the VA.
Many with PTSD also face higher risk of obstructive sleep apnea specifically, with one impacting the other.
In a study of veterans being treated for PTSD, a large number (69%) of Iraq and Afghanistan veterans were also at high risk for obstructive sleep apnea (OSA).
If you’re a veteran dealing with both, understanding how they impact each other and seeking service connection can be important in getting the VA benefits you deserve.
In this article we’ll talk about:
- How is sleep apnea and PTSD linked in veterans?
- What are the risk factors of sleep apnea in veterans?
- Steps to take to show your sleep apnea is a result of your PTSD
- What can your rating look like with both conditions connected?
- Tips on getting ready for a C&P exam to establish this connection
What is the connection between sleep apnea and PTSD in veterans?
PTSD, or Post-Traumatic Stress Disorder, is a condition that can occur in veterans after experiencing traumatic events in the military.
It often includes symptoms like nightmares, flashbacks and anxiety.
Sleep Apnea, on the other hand, is a sleep disorder where breathing during sleep repetitively stops and starts, leading to disrupted sleep cycles/sleep deprivation and various other health issues, up to and including death.
There are three types of sleep apnea:obstructive sleep apnea (OSA), central sleep apnea and mixed sleep apnea, with the most common type in veterans being OSA.
There are reasons why sleep apnea and PTSD often occur together in veterans.
Veterans with PTSD often have a higher rate of OSA due to reduced REM sleep and increased sleep disturbances.
Depression associated with PTSD can also lead to lifestyle changes such as poor eating habits or lack of exercise, which can lead to weight gain and could be associated with sleep apnea.
Additionally, if a veteran has sleep apnea, it can often make their PTSD symptoms worse.
Why do veterans get sleep apnea?
Sleep apnea is more common in the veteran population for a variety of reasons.
Some of these include:
- Trauma: Military service, especially for those who served in combat zones, can lead to post-traumatic stress (PTSD), which disrupts sleep patterns, causes sleep disturbances and increases risk of sleep apnea.
- Lifestyle Factors: Military lifestyle may involve irregular sleep schedules and exposure to situations that are stressful, both contributing to sleep disorders. Other medical conditions can also cause issues.
- Physical Health Issues: Injuries or health conditions are common among veterans, and those like obesity/weight gain or respiratory issues, can also be risk factors for sleep apnea.
- Mental Health Conditions: depression can exacerbate the physical health issues linked to OSA, anxiety can exacerbate the sleep issues linked to OSA such as disrupted REM sleep.
How do I prove my sleep apnea is secondary to my PTSD?
To prove the secondary service connection between your PTSD and sleep apnea, you’ll need to show that your sleep problems are directly linked to your PTSD, and that they were caused by your time in service.
Here’s how you can do it:
- Medical Records: Gather all health records that show your history of both your PTSD and your sleep apnea. Generally speaking, the more detail you have, the better, so you can prove you have a service-connected disability.
- Doctor’s Statement: Get a statement from your doctor or a VA medical professional. They can explain at length about why they believe your PTSD and sleep apnea are connected and related to your service.
- Sleep Study Results: If you have a sleep study done, the results are important. They can indicate how severely your sleep apnea impacts your life, which can help with rating you appropriately.
- Personal Statement: Write down your own experiences. How do you feel your PTSD affects your sleep? How do you feel during the day? Are there things you notice about its impacts on your day-to-day life?
- Buddy Statements: Statements from friends and family, as well as those who served with you, are known as “buddy statements” or “buddy letters” and can help demonstrate how others believe your sleep apnea and PTSD affect you.
Remember, the VA looks at all the information and evidence you provide them in your claim to help decide if there’s a secondary service connection between your sleep apnea and PTSD.
It’s important to give them as much as you can and in as much detail.
Want to learn more about how to provide the VA with the best evidence possible for your claim? Check out our evidence guide below.

Read about the types of evidence you need for your VA claims by clicking here!
What would my rating look like with Sleep Apnea and PTSD connected?
If your sleep apnea and PTSD have secondary service connection, your VA rating could vary, but being connected for both would likely be a benefit for you.
PTSD ratings are at 0%, 10%, 30%, 50%, 70% or 100%, with 70% being a common rating.
Sleep apnea is rated at 0%, 30%, 50% or 100%. The most common ratings tend to be 30% or 50%, with 50% requiring a prescription of a CPAP machine.
When you are rated for both of these conditions and they are combined, you will be assigned a combined VA rating.
Remember–this isn’t as simple as just adding them together.
VA math is a bit complicated, and considers the combined impact of your conditions on your life, which isn’t always a 1+1 scenario.
If you want to know how your sleep apnea and PTSD ratings might combine and affect your overall disability rating and potential compensation and disability benefits, we’ve taken the guesswork out of it for you with our VA Disability Calculator.
With our calculator, you can determine:
- Your Expected Combined Disability Rating: Get an estimate of the combined rating for your PTSD and sleep apnea without the added confusion.
- Your Potential Compensation: See what financial support from the VA you might get, based on your disability ratings.
Want to see what your VA disability rating and compensation could be for PTSD and sleep apnea? Try our calculator below.

Try our VA Disability Calculator now by clicking here!
How Can I Prepare for my C&P Exam to connect PTSD and Sleep Apnea?
Perhaps one of the most critical components of a winning VA disability claim is the often dreaded compensation and pension (C&P) exam.
When you go to this exam to connect your sleep apnea and PTSD as a secondary condition, the examiner will look closely at your health history and how both conditions affect you.
They typically will check things like:
- How well you are sleeping
- If you snore, how loudly and how it impacts your sleep
- If you have daytime sleepiness or excessively tired during the day
- If you have nightmares or flashbacks because of PTSD
- How both of these conditions impact your work and social life
They will also check your medical records for any sleep diagnostic testing.
If you have private sleep study records, it’s a good idea to bring them along.
It’s important to be honest with the examiner about all of your symptoms and how they impact your day-to-day life.
Each exam will always be a little different from the next, but to be as prepared as possible, be sure to check out our comprehensive guide below.

How do I pass my C&P the first time? Click here to find out!
Cassandra Crosby, an Accredited Agent and claims advocate for Matthew Hill & Shelly Mark’s teams, reviewed the information provided in this post.
References:
- U.S. Department of Veterans Affairs. (2022). “Annual Benefits Report Fiscal Year 2022.” VA Compensation Report.
- Colvonen, P. J., et al. (2015). “Obstructive sleep apnea and posttraumatic stress disorder among OEF/OIF/OND veterans.” Journal of Clinical Sleep Medicine.
- Veterans Health Library. “Veterans Health Library.” Accessed at Veterans Health Library.
- Sharafkhaneh, A., et al. (2022). “Association of PTSD and obstructive sleep apnea in veterans.” PubMed Central.