There are three elements needed to establish service connection for PTSD in order to receive VA benefits. First, you must have a current diagnosis of PTSD from an expert who is competent to diagnose the disorder. Second, there must be credible supporting evidence that the claimed in-service stressor actually occurred. And third, there must be medical evidence of a causal nexus between the current symptomatology and the claimed in-service stressor. The following is a flow chart that you may use in order to determine what evidence is needed to establish service connection for a variety of situations.
1: Do you have a current diagnosis of PTSD from a qualified medical expert who is competent to diagnose the disorder?
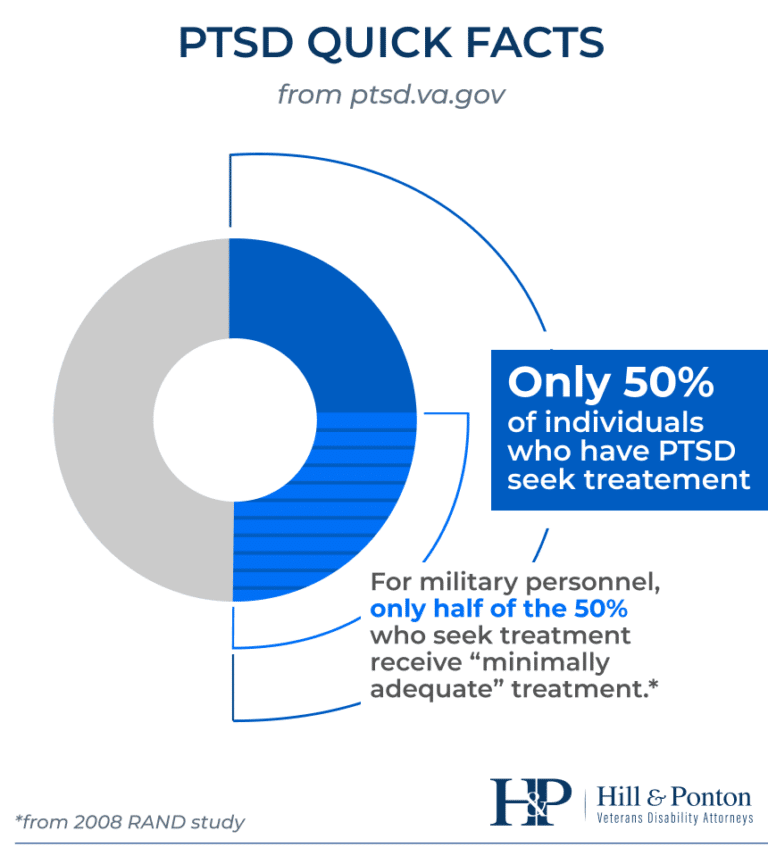
In order for the VA to recognize a veteran’s PTSD in order to award service connection, the diagnosis must be provided by a qualified medical professional. Even though many veterans are treated by VA or private therapists who are not doctors or psychologists (i.e. licensed mental health social workers, licensed counselors, etc.), the VA will not accept their opinions initially diagnosing PTSD. According to the VA Clinician’s Guide, professionals qualified to perform PTSD Compensation and Pension examinations (C&P exams) must have doctoral-level training in psychopathology, diagnostic methods, and clinical interview methods. They must have a working knowledge of the DSM-V and extensive clinical experience in diagnosing and treating veterans with PTSD. Persons with the requisite professional qualifications include board-certified psychiatrists and licensed psychologists, as well as psychiatric residents and psychology interns under the close supervision of an attending psychiatrist or psychologist. See Part Three for more specific information about C&P exams.
In addition, the diagnosis must conform to the diagnostic criteria in the DSM-V. The most common reason the VA denies a claim for PTSD is because it believes that a veteran does not meet all of the diagnostic criteria in the DSM-V for PTSD. A veteran may be suffering from extreme PTSD, but if his or her symptoms do not fall neatly within the diagnostic criteria for PTSD, then for VA purposes, the veteran does not have PTSD, and service connection will be denied. The diagnostic criteria in the DSM-V for PTSD are listed below. After the stressor criterion, there are four symptom clusters: intrusion, avoidance, negative alterations in cognitions and mood, and alterations in arousal and reactivity. The sixth criterion concerns duration of symptoms, the seventh assesses functioning, and the eighth criterion clarifies that symptoms are not attributable to a substance or co-occurring medical condition. Note that some criterions require only one symptom, while others require multiple symptoms.
Criterion A: stressor
The person was exposed to: death, threatened death, actual or threatened serious injury, or actual or threatened sexual violence, as follows: (one required)
- Direct exposure.
- Witnessing, in person.
- Indirectly, by learning that a close relative or close friend was exposed to trauma. If the event involved actual or threatened death, it must have been violent or accidental.
- Repeated or extreme indirect exposure to aversive details of the event(s), usually in the course of professional duties (e.g., first responders, collecting body parts; professionals repeatedly exposed to details of child abuse). This does not include indirect non-professional exposure through electronic media, television, movies, or pictures.
Examples: Combat participation, military sexual trauma, witnessing a roadside bomb go off a few vehicles ahead, learning that a family member was killed in a car accident, or being part of a burial crew. Note that number three above may be the most difficult way to satisfy Criterion A. For instance, if the person involved is not a “close” friend, but the veteran made a decision that put that person in a dangerous situation and the person dies, this may not be enough to satisfy Criterion A even though the veteran may be traumatized because he or she feels responsible.
Criterion B: intrusion symptoms
The traumatic event is persistently re-experienced in the following way(s): (one required)
- Recurrent, involuntary, and intrusive memories.
- Traumatic nightmares.
- Dissociative reactions (e.g., flashbacks) which may occur on a continuum from brief episodes to complete loss of consciousness.
- Intense or prolonged distress after exposure to traumatic reminders.
- Marked physiologic reactivity after exposure to trauma-related stimuli.
Criterion C: avoidance
Persistent effortful avoidance of distressing trauma-related stimuli after the event: (one required)
- Trauma-related thoughts or feelings.
- Trauma-related external reminders (e.g., people, places, conversations, activities, objects, or situations).
Criterion D: negative alterations in cognitions and mood
Negative alterations in cognitions and mood that began or worsened after the traumatic event: (two required)
- Inability to recall key features of the traumatic event (usually dissociative amnesia; not due to head injury, alcohol, or drugs).
- Persistent (and often distorted) negative beliefs and expectations about oneself or the world (e.g., “I am bad,” “The world is completely dangerous”).
- Persistent distorted blame of self or others for causing the traumatic event or for resulting consequences.
- Persistent negative trauma-related emotions (e.g., fear, horror, anger, guilt, or shame).
- Markedly diminished interest in (pre-traumatic) significant activities.
- Feeling alienated from others (e.g., detachment or estrangement).
- Constricted affect: persistent inability to experience positive emotions.
Criterion E: alterations in arousal and reactivity
Trauma-related alterations in arousal and reactivity that began or worsened after the traumatic event: (two required)
- Irritable or aggressive behavior
- Self-destructive or reckless behavior
- Hypervigilance
- Exaggerated startle response
- Problems in concentration
- Sleep disturbance
Criterion F: duration
Persistence of symptoms (in Criteria B, C, D, and E) for more than one month.
Criterion G: functional significance
Significant symptom-related distress or functional impairment (e.g., social, occupational).
Criterion H: exclusion
Disturbance is not due to medication, substance use, or other illness.
Specify if: With dissociative symptoms.
In addition to meeting criteria for diagnosis, an individual experiences high levels of either of the following in reaction to trauma-related stimuli:
- Depersonalization: experience of being an outside observer of or detached from oneself (e.g., feeling as if “this is not happening to me” or one were in a dream).
- Derealization: experience of unreality, distance, or distortion (e.g., “things are not real”).
Specify if: With delayed expression.
Full diagnosis is not met until at least six months after the trauma(s), although onset of symptoms may occur immediately.
Sometimes, the VA will reject a competent diagnosis of PTSD because the diagnosis is not “clear” – this is an incorrect legal standard and an appealable issue. Instead, for this first element of service connection for PTSD, the diagnosis must detail whether it is “as likely as not” that the veteran is currently suffering from PTSD. In addition, the VA cannot reject a competent diagnosis of PTSD without providing an adequate statement of reasons or bases for its decision. The VA must also be able to point to other medical evidence in the record to support its conclusion that the veteran is not currently suffering from PTSD, in other words VA cannot state that a veteran does not have PTSD simply because it does not believe the veteran’s doctor.
If you have a current diagnosis of PTSD from an expert who is competent to diagnose the disorder, move on to step 2.
NOTE: The DSM-V was published on May 18, 2013, but was not adopted in the Code of Federal Regulations until August 4, 2014 (79 F.R. 45093). The DSM-V will be used for all claims that were received by the VA or pending at the regional office level on August 4, 2014, but the rule change does not apply to claims that have been certified for appeal to the Board of Veterans’ Appeals or are pending before the Court of Appeals for Veterans Claims or the Court of Appeals for the Federal Circuit. Therefore, some PTSD cases will still be evaluated using the DSM-IV criteria.
2: Do you have credible supporting evidence that the claimed in-service stressor actually occurred?
This element of establishing service connection for PTSD is the stumbling block for many veterans, but even if you are doubtful that you will be able to corroborate your stressor, hope is not lost. Use the following flowchart to determine what evidence is needed for your claim.
Was the veteran diagnosed with PTSD during a period of active military service?
PTSD Diagnosed During Active Military Service
If a veteran is diagnosed with PTSD during a period of active military service, there is a lower burden of proof for stressor corroboration evidence. If the claimed stressor is related to that service, the stressor is consistent with the circumstances of that service, and there is no clear and convincing evidence to the contrary, the veteran’s own statements may be used to establish the occurrence of the claimed stressor. The lower burden of proof applies to claims pending on or filed after October 29, 2008.
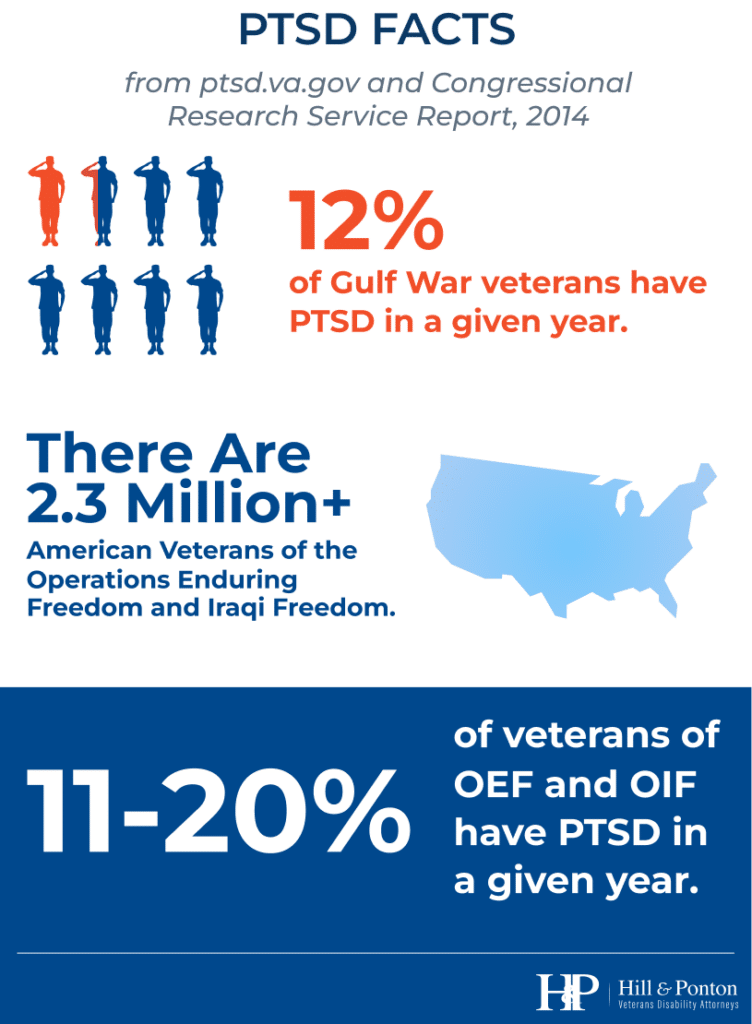
Another important thing to note is that if a veteran is released from service because of a mental disorder that developed as a result of a highly stressful event in service, the veteran must be awarded a disability rating of not less than 50 percent and be scheduled for a reevaluation within 6 months.
Is the stressor related to fear of hostile military or terrorist activity?
PTSD Related to Fear of Hostile Military or Terrorist Activity
A veteran who is diagnosed with PTSD that is related to fear of hostile military or terrorist activity does not need to provide stressor corroboration evidence as long as a VA psychologist or psychiatrist has diagnosed the PTSD and says that the stressor is related to the veteran’s fear of hostile military or terrorist activity. If a veteran’s stressor is adequate to support a diagnosis of PTSD, that stressor is consistent with the circumstances of the veteran’s service, and there is no clear and convincing evidence to the contrary, the veteran’s own statements may be used to establish the occurrence of the claimed stressor.
What is fear of hostile military or terrorist activity? The veteran must have experienced, witnessed, or been confronted with an event or circumstance that involved actual or threatened death or serious injury, or a threat to the physical integrity of the vet or others, such as from an actual or potential improvised explosive device; vehicle-embedded explosive device; incoming artillery, rocket, or mortar fire; grenade; small arms fire, including suspected sniper fire; or attack upon friendly military aircraft, and the veteran’s response to the event or circumstance must have involved a psychological or psycho-physiological state of fear, helplessness, or horror.
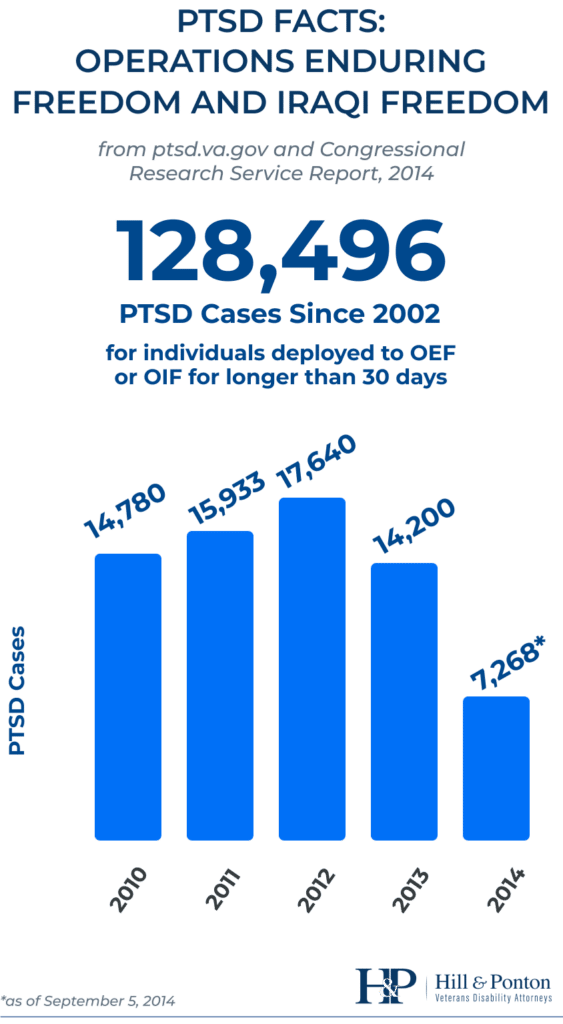
This lower burden of proof applies to all veterans, regardless of where they experience the fear of hostile military or terrorist activity, but it does not include sexual assault or hostile criminal actions of US military personnel directed against other US military personnel. It also only applies to claims received on or pending after July 13, 2010. If a veteran has a previously denied PTSD claim, in order to reopen the claim under this lower burden of proof standard, he or she would need a lay statement of his or her fear of hostile military or terrorist activity and service records that show service in an area involving exposure to hostile military or terrorist activity.
It is important to note that while this lower burden of proof requires a diagnosis by a VA psychologist or psychiatrist, a diagnosis by a non-VA practitioner and a veteran’s statement describing an in-service stressor relating to a fear of hostile military or terrorist activity should be enough to trigger the VA’s duty to assist by scheduling a VA PTSD exam.
NOTE: If a veteran is attempting to get service connection for PTSD under this lower burden of proof standard, but the VA psychologist or psychiatrist’s opinion states that the doctor does not believe that the veteran’s PTSD is related to a fear of hostile military or terrorist activity, the veteran should attempt to gather corroborating evidence of the stressor, which another doctor can use as a basis for a medical nexus opinion under step 3.
Did the claimed stressor occur during combat?
PTSD for Combat Veterans
Similar to veterans who were diagnosed with PTSD during service, there is a lower burden of proof for combat veterans when it comes to stressor corroboration evidence. Essentially, the VA admits that when a veteran is engaged in combat, his or her primary focus is going to be carrying out the mission, not taking notes on any and all injuries. If a veteran’s stressor is related to combat, that stressor is consistent with the circumstances of the veteran’s service, and there is no clear and convincing evidence to the contrary, the veteran’s own statements may be used to establish the occurrence of the claimed stressor.

The VA Adjudications Procedures Manual M21-1MR defines combat as “personal participation in events constituting an actual fight or encounter with a military foe or hostile unit or instrumentality. It includes presence during such events either as a combatant, or service member performing duty in support of combatants, such as providing medical care to the wounded.” Even a brief participation in combat triggers the lower burden of proof. But, depending on the circumstances, it is important to note that the veteran may have an additional hurdle in proving that he or she was in combat.
For some veterans, this is a simple task due to their military service records or military occupational specialty (MOS) and where or when they served. But for other veterans, it may not be obvious at first glance that they served in combat. For these veterans, the VA will look to not only military service records and MOS, but also certain military decorations, buddy statements, letters home to family or friends, copies of newspapers or regimental or divisional newsletters, photographs, or any other credible supporting evidence that can help to establish whether the veteran was in combat or not. If a veteran contends that he was in combat action that cannot be confirmed by his or her MOS or military service records, the VA must make a finding as to the credibility of his or her statement and provide reasons for its finding of whether the veteran engaged in combat, keeping in mind the benefit of the doubt rule.
At this stage, if a veteran states that he served in combat and identifies a stressor that is not impossible to believe, and has a current diagnosis of PTSD (see step 1), then the VA must take steps to develop evidence. The VA will look for evidence of both combat service and additional evidence that the combat stressor actually took place. It is usually a good idea for the veteran to request these records as well. Relevant service records may be found at the National Personnel Records Center, the US Army and Joint Services Records Research Center, the Marine Corps Archives and Special Collections, and the National Archives.
Once it is established that the veteran served in combat, the VA must also accept lay evidence as proof that the alleged stressor happened during combat even in the absence of official records or supporting clinical evidence. Even if the veteran does not have any other evidence that the stressor occurred other than his or her own statement, as long as there is not clear and convincing evidence to the contrary, the VA is obligated to apply the benefit of the doubt rule and accept the veteran’s own statement as proof that the stressor occurred.
Is the stressor related to an in-service personal assault or trauma, including Military Sexual Trauma (MST)?
Special rules for in-service personal assault or trauma as stressor
If a veteran suffers from PTSD as a result of an in-service personal assault or trauma such as rape, physical assault, domestic battering, robbery, mugging, stalking, or harassment, the stressor can be corroborated through alternative evidence if military records do not document that a personal assault occurred. The VA has a special obligation to assist in these cases (commonly referred to as Military Sexual Trauma or MST) and must inform the veteran that evidence other than that found in service records may be submitted. Alternative sources for evidence may be things such as records from law enforcement, rape crisis centers, mental health counseling centers, hospitals, or physicians; pregnancy or STD tests; statements from family members, roommates, fellow service members, or clergy; a personal diary or journal; or evidence of behavior changes such as a request to transfer, deterioration in work performance, substance abuse, depression, panic attacks, or anxiety. Unfortunately, these cases are frequently denied, partly due to the fact that VA has difficulty compensating for disabilities that are less obvious than a physical disability such as PTSD and depression, and because due to the nature of MST cases it is rare for there to be a formal report or complaint in the record. The VA often must rely on the alternative evidence listed above, and typically fails to give that evidence the weight that is required. PTSD claims in general are difficult to win, but VA MST claims are even tougher.
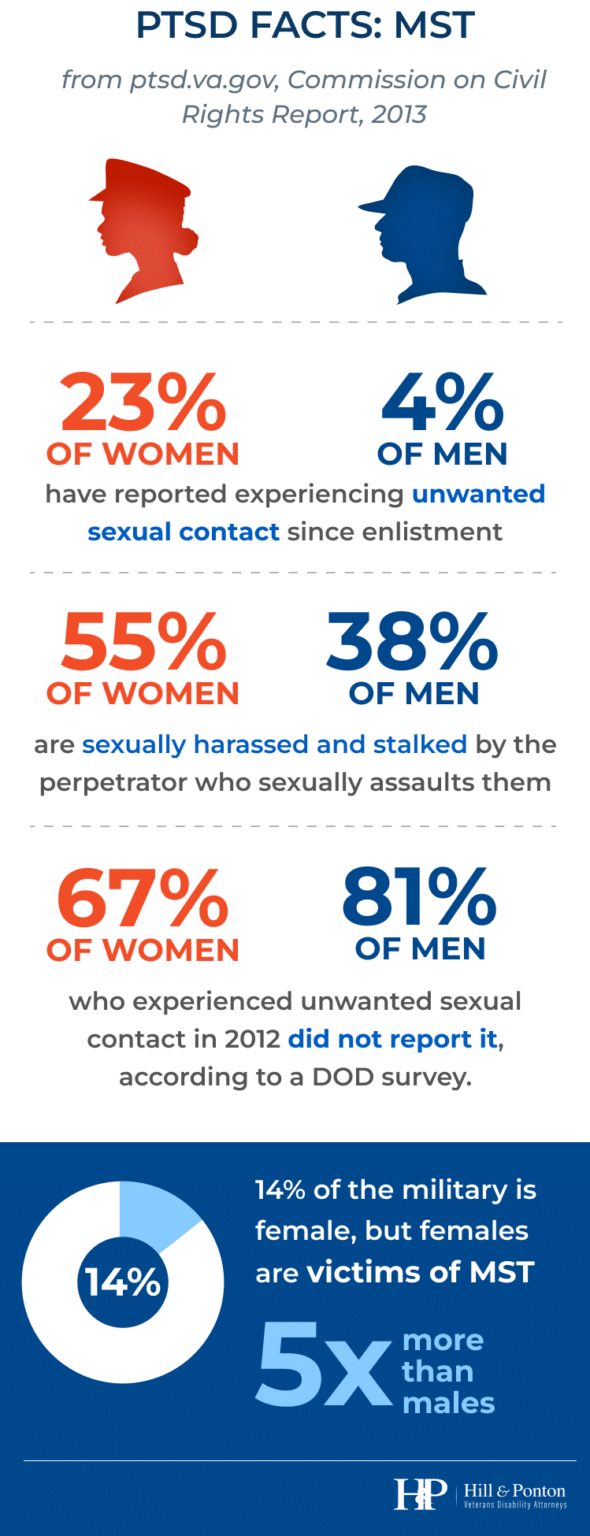
Another hurdle identified in the GAO report is the variation in the thoroughness of C&P examinations for MST claims. In fact, during the only formal training for VA examiners who are conducting MST exams, less than 5% of the one-hour certification course for PTSD examiners is devoted to MST. This goes to show that there is still a lot of work and training that needs to be done on the VA side in regards to MST claims, which can be discouraging for many veterans. But just remember that while MST claims take time, they are not impossible to win. The key is to get the VA to look at the stressor evidence in the right context in order to show, for example, a behavior change that corroborates the occurrence of the stressor. See Part Seven for a list of resources for survivors of MST.
According to a June 2014 report from the Government Accountability Office, since 2008, there have been 29,000 veterans who have sought disability benefits for problems related to MST. PTSD is the most common disability claimed as a result of MST at 94 percent of claims, with major depressive disorder and anxiety disorder being the second and third most common. The overall approval rating for PTSD related to MST is up from 28 percent in 2010 to roughly 50 percent in 2013, but this is still lower than the 55 percent approval rating for other forms of PTSD
Note: According to a report by the ACLU and Service Women’s Action Network, between 2008 and 2012, the award of MST-related PTSD claims was lower than the rate of other PTSD claims by between 16.5 and 29.6 percent each year). Also of note is the wide disparity among regional offices: in some ROs as few as 14 percent of claims were approved, while other ROs approved as many as 88 percent of claims. The GAO report found that regional offices are having ongoing difficulty applying broadened MST standards and may differ wildly in their interpretations of the evidence in the claim file.
If none of the above applies, stressor corroboration is needed
If a veteran’s claim for PTSD does not fit into one of the above categories, there must be evidence that corroborates the occurrence of the stressor, meaning credible supporting evidence that the claimed in-service stressor occurred. The supporting evidence must include more than the veteran’s own testimony. Unless there is no reasonable possibility that assistance by the VA would aid in substantiating the claim, the VA must assist the veteran in developing evidence that supports the existence of a stressor.
For the veteran’s service records to corroborate the stressor, they do not need to include every detail of the event. If there is independent evidence of the occurrence of a stressful event and that evidence shows the veteran’s personal exposure to the event, that could be sufficient corroborative evidence. In addition, credible supporting evidence can come from lay sources such as buddy statements.
An example of a situation in which a veteran would need stressor corroboration evidence is if he or she was in a bad car accident during service, the car accident was not related to combat, and the veteran was not diagnosed with PTSD until after leaving service. In this situation, the veteran would need to be able to corroborate that the car accident happened. This may be through a police report, hospital records, statements of the other individuals involved in the accident, or other supporting evidence. Another situation in which corroboration evidence would be required is if a veteran was involved in an accident during a non-combat situation, such as an explosion or fire. Again, hospital records, notations in service records, and statements of other persons who witnessed the explosion would be helpful corroboration evidence.
It is important to note that if a veteran’s account of an event is contradicted by official records, the VA can reject the veteran’s account, but as long as the veteran produces evidence to back up his or her story, the benefit of the doubt rule still applies.
3. Does the Veteran have Medical Evidence of a Causal Nexus Between the Current Symptomatology and the Claimed In-Service Stressor
The final step of establishing service connection for PTSD is proving a causal nexus between the current symptomatology and the claimed in-service stressor. This step requires an opinion by a medical expert. The evidence must show that the stressor was at least a contributory basis for the current symptoms. As long as there is a clear relationship between the stressor encountered in service and the current diagnosis of PTSD, a veteran whose service medical records show no evidence of a mental disorder can be entitled to service connection for PTSD, even if the PTSD develops many years after service.
Note that this step can be more complicated if a veteran has more than one stressor. For example, say a veteran was in a car accident in service in which his best friend was killed, and there are service records and hospital records backing up this stressor. The second stressor was when the vet was in his bunk and some fellow soldiers came in the room and threw a grenade at him. The grenade was a dummy, but the veteran did not know that, and he still has nightmares about it. There is no independent verification of this stressor. For the veteran to receive service connected compensation for his PTSD, the doctor would have to relate his PTSD specifically to the car accident in service because that is the only stressor with independent verification, and the second stressor does not qualify under one of the lower burden of proof situations mentioned in step 2. And remember, the VA will always send the veteran to a Compensation and Pension exam to determine if the veteran is entitled service connected disability benefits for his PTSD.
Proceed to Part 3: Compensation and Pension Exams for PTSD