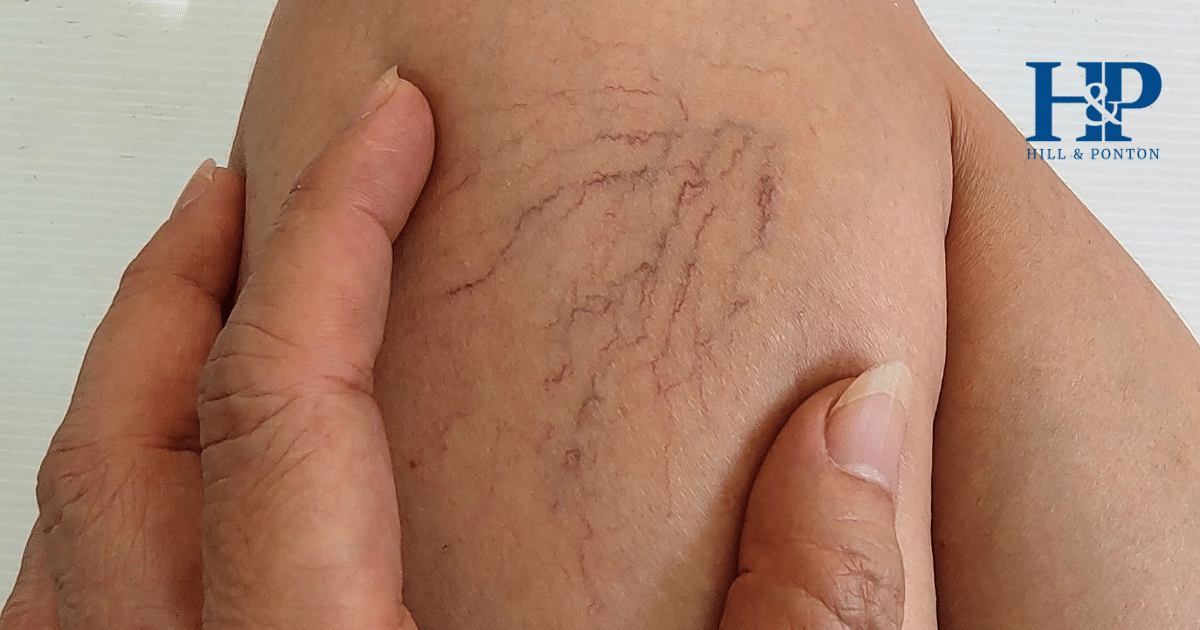
Varicose veins are a common condition among veterans, especially those who have served in physically demanding roles or experienced prolonged periods of standing. The enlarged, swollen veins often cause pain, discomfort, and other complications, significantly impacting a veteran’s quality of life. Fortunately, the VA recognizes varicose veins as a condition that may qualify for compensation. Here’s how you can obtain a VA rating and disability benefits.
What Is the VA Rating for Varicose Veins?
Under Diagnostic Code 7120, the VA disability rating for varicose veins is 0%, 10%, 20%, 40%, 60% or 100%, depending on the severity of symptoms and their impact on a veteran’s ability to function in daily life.
- 0% Rating: Asymptomatic palpable or visible varicose veins
- 10% Rating: Intermittent edema of extremity or aching and fatigue in leg after prolonged standing or walking, with symptoms relieved by elevation of extremity or compression hosiery
- 20% Rating: Persistent edema, incompletely relieved by elevation of extremity, with or without beginning stasis pigmentation or eczema
- 40% Rating: Persistent edema and stasis pigmentation or eczema, with or without intermittent ulceration
- 60% Rating: Persistent edema or subcutaneous induration, stasis pigmentation or eczema, and persistent ulceration
- 100% Rating: Massive board-like edema with constant pain at rest
Note: These evaluations are for involvement of a single extremity. If more than one extremity is involved, evaluate each extremity separately and combine (under § 4.25), using the bilateral factor (§ 4.26), if applicable.
Get Help With Your VA Disability Claim
These ratings reflect the impact varicose veins have on a veteran’s daily life, with higher ratings indicating more severe symptoms and greater impairment.
If you are experiencing varicose veins due to your military service, understanding how the VA rates this condition can help you receive the benefits you deserve. Contact us today for a free case evaluation to determine your eligibility for VA disability compensation.
How To Get Disability for Varicose Veins
To receive a VA disability rating for varicose veins, you must establish a service connection for your condition. This means proving that your varicose veins are linked to your military service, whether they were caused or aggravated by it.
Here are the steps you can take to establish service connection:
- Current Diagnosis: Obtain a current diagnosis of varicose veins from a qualified medical professional.
- In-Service Event: Provide evidence of an in-service event, injury, or illness that could have caused or aggravated your varicose veins. This could include documentation of prolonged standing, heavy lifting, or other physical activities during service.
- Medical Nexus: Secure a medical nexus opinion linking your current varicose veins to the in-service event. This opinion should come from a medical professional who has reviewed your service records and medical history.
By gathering and presenting this evidence, you can strengthen your claim and improve your chances of receiving a favorable disability rating.
Getting Help with Your VA Claim
Navigating the VA disability claims process can be challenging. Veterans who struggle to get the benefits they deserve may find it helpful to seek assistance from experienced VA disability attorneys or accredited representatives. These professionals can help you:
- Prepare Your Claim: Ensure all necessary evidence and documentation are included.
- File Appeals: If your claim is denied or you receive a lower rating than expected, they can assist with the appeals process. Ask for a free case review here.
- Maximize Benefits: Work to secure the highest possible rating for your condition.
Winning a 40% VA Disability Rating for Venous Vein Insufficiency: Case Example
In this case, a veteran who served in the U.S. military from June 1991 to June 1996 filed a claim for disability benefits due to venous vein insufficiency of both lower extremities. Initially, the veteran received a 20% disability rating for each lower extremity but believed their symptoms were more severe than reflected in the rating. After appealing the decision, the Board of Veterans’ Appeals reviewed the evidence.
The Board ultimately decided to increase the initial disability rating to 40% for both the left and right lower extremities for the entire appeal period. This decision recognized the veteran’s persistent symptoms of edema and stasis pigmentation as warranting a higher level of disability benefits under Diagnostic Code 7199-7120.
How This Claim Was Won
- Detailed Medical Evidence: The veteran’s case was supported by extensive medical records, including private treatment notes from Dr. Imtiaz Ahmad and VA examination reports. These records documented the veteran’s symptoms of persistent edema, stasis pigmentation, and venous insufficiency over time, which were crucial in meeting the criteria for a 40% disability rating.
- Consistent Symptom Documentation: The veteran consistently reported symptoms such as swelling, pain, and heaviness in the legs, along with the need to wear compression stockings daily. This continuous record of the impact of venous vein insufficiency on the veteran’s daily life played a significant role in the Board’s decision to grant a higher rating.
- Testimony and Personal Statements: Both the veteran and Dr. Ahmad provided compelling testimony at multiple hearings, detailing the severity of the veteran’s condition. Dr. Ahmad described the condition as severe, involving both superficial and deep venous insufficiency, and emphasized the ongoing need for treatment and surgery.
This case underscores the importance of comprehensive and consistent medical documentation when appealing a VA disability rating. Veterans facing similar situations should ensure that their medical records accurately reflect the severity of their condition and that they maintain thorough documentation of their symptoms.
If your rating for varicose veins is too low or your condition has worsened, request a free evaluation of your case. A well-documented appeal can make all the difference in securing the benefits you deserve.
Get Help With Your VA Disability Claim
Unhappy with your VA rating? We can help! Contact us for a free review of the case.