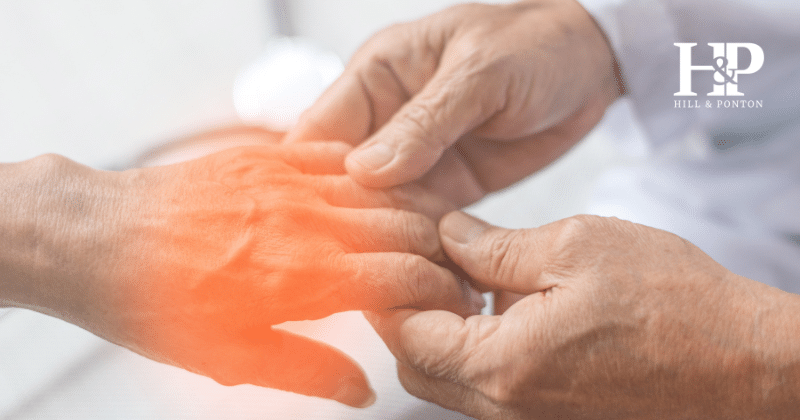
Peripheral neuropathy is a common condition and former military service members who are living with it may be eligible for VA disability ratings from 10% to 40%. In this quick guide, we’re going over the VA rating criteria for peripheral neuropathy, the connection with Agent Orange and how to obtain disability benefits.
What Is the VA Disability Rating for Peripheral Neuropathy?
Peripheral neuropathy is rated by the VA using diagnostic codes and criteria for the specific nerves affected, typically with ratings from 10% (mild nerve paralysis) to 40% for each extremity affected and the possibility of higher combined ratings for severe cases affecting multiple limbs. Peripheral neuropathy in the legs is rated the same way as the paralysis of the sciatic nerve (diagnostic code 8520), with ratings ranging from a minimum of 10% to a maximum of 80%.
- 10% – Mild
- 20% – Moderate
- 30% – Severe, with marked muscular atrophy
- 40% – Complete nerve paralysis with foot drop, inability to move the muscles below the knee, flexion of knee weakened or (very rarely) lost
To qualify for service-connected benefits, veterans must demonstrate their symptoms align with VA criteria for nerve damage. The condition will be rated based on the diagnostic code for the damaged nerves (peroneal, sciatic, femoral, etc.) and considering factors like foot drop, toe movement impairment, and sensory loss. Veterans should communicate all symptoms to their physician for an accurate assessment.
Types and Causes of Neuropathy
Neuropathies are typically classified according to the problems caused or the root of the damage.
- Mononeuropathy is damage to a single peripheral nerve. Physical injury or trauma is the most common cause. Mononeuropathy can also be caused by prolonged pressure on the nerve, extended sedentary periods or continuous repetitive motions. Carpal tunnel is a common type of mononeuropathy caused by overuse strain on the nerve that passes through an individual’s wrist. The damage can cause numbness, tingling, pain, and unusual sensations in the first three fingers on the thumb side of a person’s hand.
- Polyneuropathy is damage to multiple peripheral nerves throughout the body. It makes up the greatest number of peripheral neuropathy cases. Polyneuropathy has a wide variety of causes which include exposure to toxins such as Agent Orange or volatile organic compounds (such as those in the water at Camp Lejeune).
Common Causes of Peripheral Neuropathy in Veterans
Acquired neuropathies are caused by environmental factors (and are what a veteran would attempt to get service connected). Environmental factors which could cause neuropathy are toxins, trauma, illness, and infection. Know causes include:
Peripheral Neuropathy Presumptive to Agent Orange Exposure
Peripheral neuropathy is recognized by the VA as a condition linked to Agent Orange exposure. Veterans who were exposed to Agent Orange and developed early-onset peripheral neuropathy may qualify for presumptive service connection, meaning they don’t have to prove the condition is directly related to their military service.
To qualify for peripheral neuropathy Agent Orange compensation, the condition must have appeared within one year of exposure and be rated at least 10 percent disabling under VA regulations.
Can Agent Orange Cause Neuropathy Later In Life?
Yes. Recent changes to VA rules removed the requirement that neuropathy must resolve within two years. This means veterans with persistent neuropathy after exposure may still be eligible for compensation.
If you served in Vietnam, the Korean DMZ, or other areas where Agent Orange was used, you may also be eligible for a free Agent Orange Registry Health Exam to assess your condition.
If you’ve been denied peripheral neuropathy Agent Orange benefits, or believe your rating is too low, get in touch to see if we can assist you in receiving the compensation you’re entitled to.
Maximize Your Benefits
Unhappy with your VA decision? We’re here to help. Contact us for a free review of your case.
VA Benefits for Delayed Onset Peripheral Neuropathy
Misdiagnosis or undiagnosed peripheral neuropathy often stems from:
- Medical professionals not thoroughly listening to veterans’ nerve pain complaints.
- Failure to conduct essential diagnostic tests.
- Overlooking delayed-onset neuropathy that appears years post-service.
- Budget or time constraints affecting quality of care.
These issues can prevent veterans from accessing deserved benefits. It’s vital for veterans to insist on comprehensive medical evaluations and the necessary tests for an accurate diagnosis and assessment of neuropathy’s severity.
How Do You Prove Peripheral Neuropathy to VA?
To prove peripheral neuropathy to the VA, it’s essential to have thorough medical documentation and ensure that your condition is well-substantiated through diagnostic tests. Veterans filing a claim should consider the following steps:
- Addressing Common Challenges: Many veterans face challenges in getting a diagnosis for peripheral neuropathy, particularly due to underreported symptoms, the intermittent nature of the condition, or assumptions that these symptoms are just a part of aging. Ensure that your healthcare provider thoroughly documents your symptoms during each visit and clarifies that your condition is not related to aging but rather your military service or a service-related condition.
- Comprehensive Medical Documentation: Provide detailed medical records that outline your symptoms, including numbness, tingling, pain, and loss of muscle strength. Diagnostic tests such as electromyography (EMG), nerve conduction velocity tests (NCV), and even nerve biopsies are crucial in showing the extent and persistence of your peripheral neuropathy. Ensure that these documents are updated and clearly show the progression of the condition over time.
- Symptom Diary: Keep a daily log of your symptoms, detailing the severity, frequency, and how it impacts your daily activities. This can provide a clearer picture of how peripheral neuropathy affects your quality of life.
- Medical Opinions: A strong medical opinion from a healthcare provider that links your peripheral neuropathy to your service or to another service-connected condition is crucial. The physician should explain how the neuropathy is related to your military service or a service-related injury.
Many veterans who are service connected for other disabilities also suffer from peripheral neuropathy; however, they have never been formally diagnosed with this condition.
How To Prove Peripheral Neuropathy Secondary to Diabetes
Veterans receiving VA compensation for Diabetes Mellitus may also qualify for disability compensation for conditions secondary to diabetes. Diabetic neuropathy, a common microvascular complication, manifests as nerve damage over time due to prolonged high glucose levels damaging the blood vessels that support nerves.
Diabetic Neuropathy Types:
- Peripheral neuropathy (most common, affecting extremities)
- Autonomic neuropathy (affects the autonomic nervous system, impacting internal organs)
- Proximal neuropathy (impacts hips, buttocks, thighs)
- Focal neuropathy (targets specific nerves or nerve groups)
Veterans should seek a medical diagnosis and present records to the VA to potentially receive additional disability benefits for secondary conditions related to diabetes, including various types of neuropathy.